PRP vs Cortisone: Which Is Right for You?
Comparing two popular injection therapies for joint pain and inflammation.
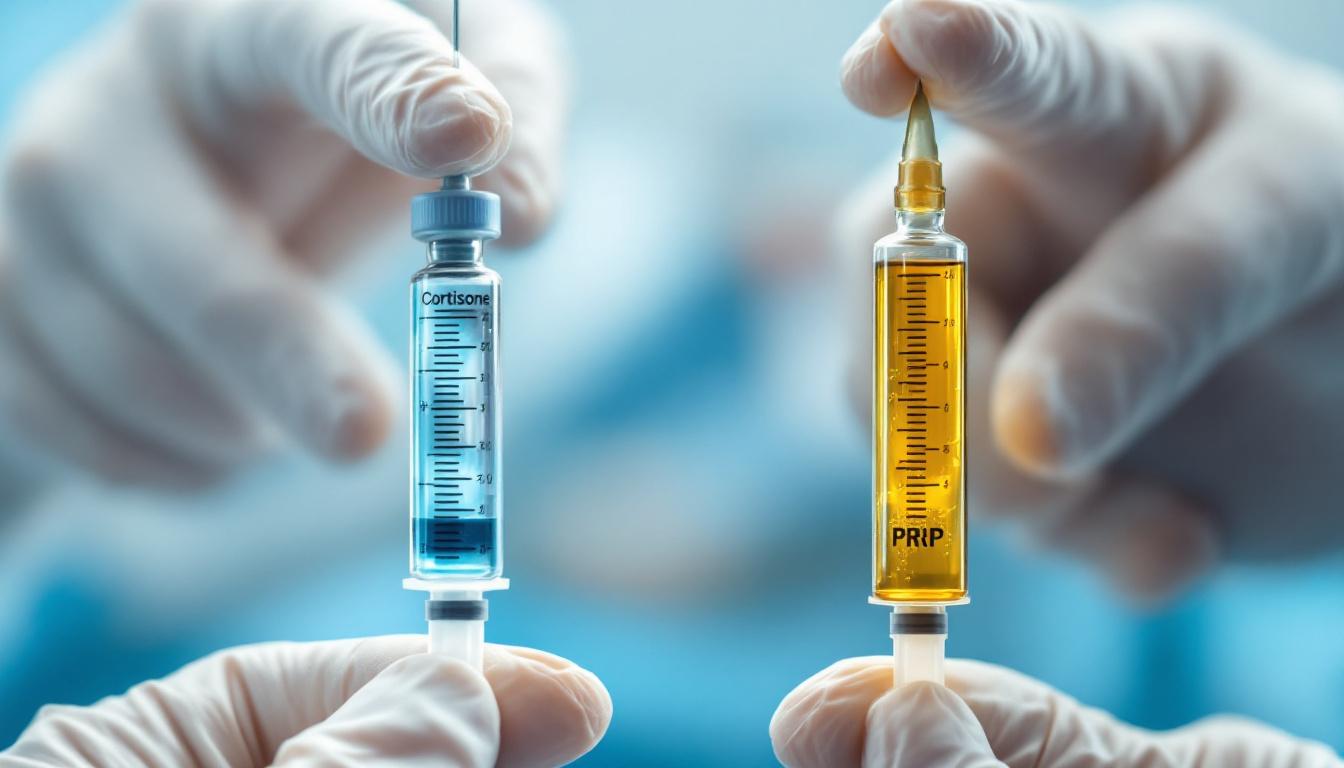
How Corticosteroid Injections Work
| Factor | PRP Therapy | Cortisone Injection | Clinical Significance | Patient Consideration |
|---|---|---|---|---|
| Mechanism | Growth factor-driven tissue regeneration | Anti-inflammatory corticosteroid suppression | PRP addresses root cause; cortisone manages symptoms | PRP preferred for long-term repair; cortisone for rapid flare relief |
| Onset of Relief | 4–8 weeks (gradual) | 1–3 days (rapid) | Cortisone wins for speed; PRP wins for durability | Time-sensitive events may favor cortisone short-term |
| Duration of Effect | 12–24+ months | 6–12 weeks | PRP provides significantly longer-lasting benefit | PRP more cost-effective over multiple treatment cycles |
| Tissue Effects | Stimulates collagen synthesis and repair | Can weaken tendons and cartilage with repeated use | PRP safer for structural integrity over time | Cortisone use >3 injections per year not recommended |
| Insurance Coverage | Typically not covered; $500–$2,500 per injection | Usually covered; low out-of-pocket cost | Cortisone lower upfront cost; PRP better long-term value | Budget and coverage should be discussed with provider |
How PRP Works Differently

What Head-to-Head Research Shows
The Risks of Repeated Corticosteroid Use
When to Choose PRP Over Cortisone
Sources
Frequently Asked Questions
Talk to a PRP Specialist About Your Options
An experienced orthopedic provider can help you decide between PRP and cortisone based on your specific condition and goals.
Find a PRP ProviderRelated Articles
Back to the Trails: A Runner's PRP Success Story
How one marathon runner returned to competition after PRP treatment for plantar fasciitis.
Does Insurance Cover PRP Injections? What Patients Need to Know
Most insurance plans don't cover PRP therapy yet. Learn why, which exceptions exist, and how to use HSA/FSA funds or financing to manage the cost.
How Long Do PRP Injections Last? What the Research Shows
PRP results can last 6 months to 2+ years depending on the condition and patient. Here's what clinical research says about PRP longevity and when to repeat treatment.
How Many PRP Injections Do You Need? A Treatment Planning Guide
Most patients need 1 to 3 PRP injections. Learn the standard treatment protocols by condition, what affects how many shots you need, and when to consider a second course.
How Much Does PRP Therapy Cost? A Complete 2026 Guide
Wondering what PRP therapy costs in 2026? Learn average prices by treatment area, what drives the cost, and how to make PRP affordable without insurance.
My PRP Journey: From Chronic Pain to Active Living
One patient shares their experience with PRP treatment for a rotator cuff injury.
New Research Shows PRP Effective for Knee Osteoarthritis
A comprehensive meta-analysis reveals promising outcomes for patients with moderate knee arthritis.
Preparing for Your First PRP Injection
Tips and guidelines to help you prepare for a successful PRP treatment session.
PRP as an Alternative to Joint Replacement Surgery: Who Qualifies?
Can PRP therapy help you avoid knee or hip replacement? Learn who qualifies for PRP as an alternative to surgery, what the evidence shows, and when surgery becomes necessary.
PRP Injection Recovery: What to Expect in the Days and Weeks After
What should you expect after a PRP injection? Here's a complete recovery timeline covering pain, activity restrictions, and tips that speed healing.
