Elbow bursitis, olecranon bursitis, causes painful swelling at the bony tip of the elbow that can persist for months despite aspiration and conservative care. Corticosteroid injections reduce swelling quickly but carry a meaningful risk of bursal infection and skin atrophy in this superficial location. PRP (Platelet-Rich Plasma) is an emerging alternative for chronic or recurrent olecranon bursitis: direct RCT evidence for this specific condition is limited, but the biological rationale is sound and clinical evidence from adjacent bursitis conditions supports PRP's role as a durable, lower-risk option for patients who have failed or want to avoid repeat cortisone.
What Is Elbow Bursitis?
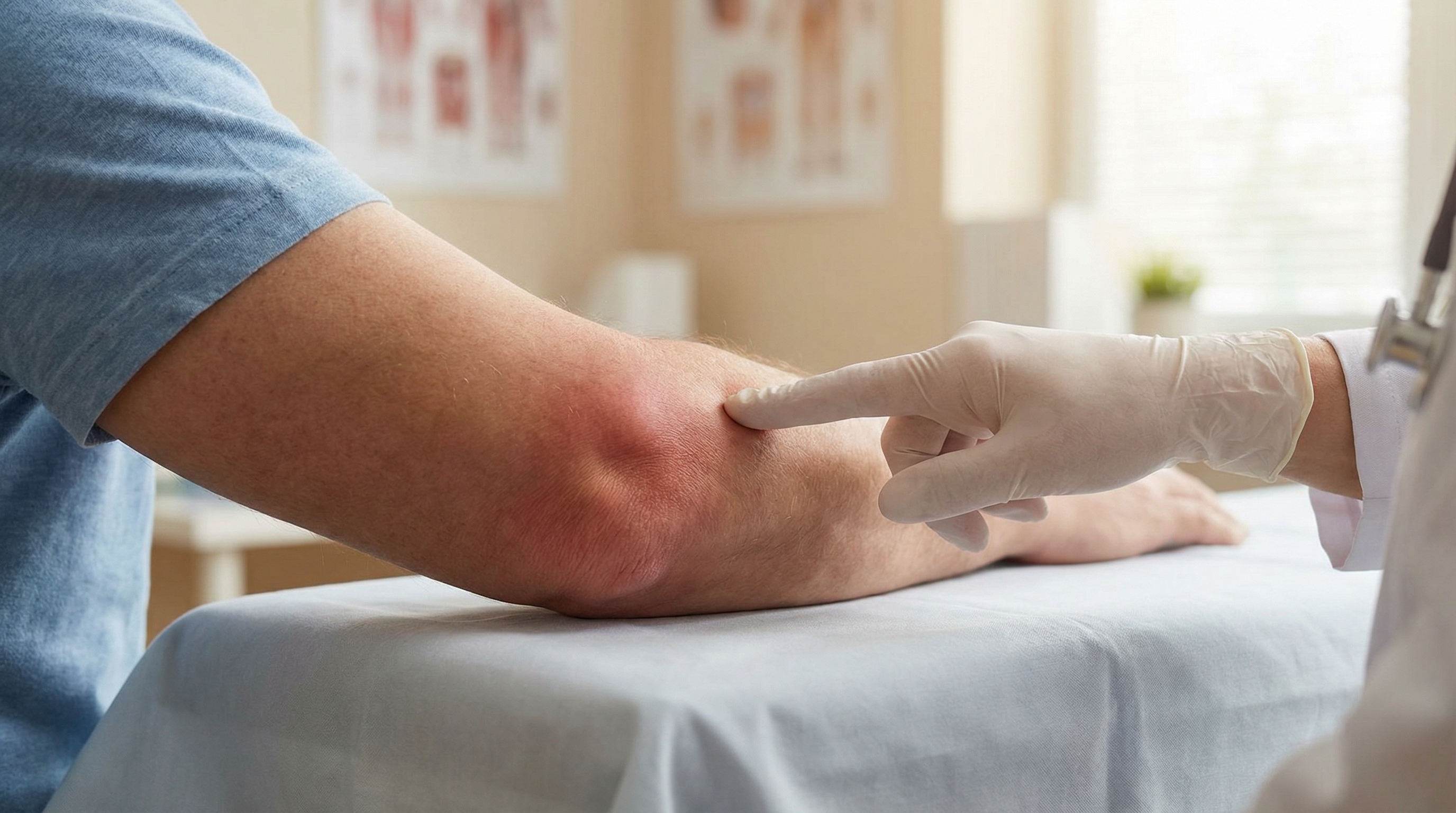
The olecranon bursa is a small fluid-filled sac that sits over the bony prominence at the back of the elbow, the olecranon. Its job is to cushion and reduce friction between the skin and the olecranon process. When the bursa becomes inflamed, it fills with fluid and produces the characteristic swelling: a soft, rounded lump at the elbow tip that can range from mildly tender to acutely painful.
Olecranon bursitis develops after prolonged pressure on the elbow (occupational or habitual leaning), direct trauma, inflammatory conditions (gout, rheumatoid arthritis), or without a clear cause. Septic (infected) bursitis requires antibiotic treatment and sometimes drainage, injection therapy is not appropriate until infection is excluded. Aseptic (non-infectious) olecranon bursitis is the target for conservative and injection-based treatments.
The olecranon bursa is uniquely superficial, it sits just beneath the skin, with minimal tissue protection. This anatomy makes cortisone injections effective but risky: the superficial location significantly increases the risk of infection, skin atrophy, and cutaneous sinus formation compared to deep bursal injections elsewhere. These risks are clinically meaningful and factor into treatment decisions for patients with chronic or recurrent disease.
Initial management includes aspiration, protective padding, activity modification, and NSAIDs. For persistent or recurrent bursitis, corticosteroid injection is the standard next step. For patients who have had cortisone with incomplete or short-lived benefit, or who have concerns about infection or repeat steroid exposure, PRP is a biologically rational alternative.
How PRP Works for Elbow Bursitis
PRP for olecranon bursitis is injected directly into the bursal space under ultrasound guidance. The concentrated platelet growth factors, PDGF, TGF-β, IGF-1, and VEGF, work to resolve the chronic inflammatory state within the bursal tissue and activate fibroblasts to produce collagen and support structural repair. The goal is to correct the underlying biology driving chronic bursal thickening and fluid accumulation, not simply suppress inflammation temporarily.
Ultrasound guidance allows the provider to visualize the bursa in real time, confirm fluid is present, and guide the needle into the bursal space accurately. Because the olecranon bursa is superficial, ultrasound also allows monitoring of the needle tip close to the skin surface, important for avoiding inadvertent subcutaneous or intradermal injection, which can cause soft-tissue damage at this thin-skinned location.
Unlike cortisone, PRP does not carry risks of skin atrophy, hypopigmentation, or infection from a steroid vehicle. For patients in whom these cortisone-related complications are a concern, particularly those who have had previous cortisone injections at this site or who have thin overlying skin, PRP avoids these risks while still delivering a biologically active treatment directly to the bursa.
What the Research Shows
Dedicated randomized controlled trial evidence for PRP in olecranon bursitis is currently absent from the medical literature. The condition itself has a limited clinical trial base, even for conventional treatments. A
2023 systematic review of non-surgical treatment for aseptic olecranon bursitis1, published in Reumatología Clínica, identified only 4 studies meeting inclusion criteria (2 RCTs, 2 observational) and found that clinical resolution can occur with conservative methods, while corticosteroid injection accelerates symptom resolution but carries a higher rate of complications including bursal infection and skin atrophy. PRP was not examined.
The most directly applicable bursitis PRP evidence comes from subacromial bursitis research. A
2024 double-blind randomized controlled trial of 100 patients with subacromial bursitis2, published in the Journal of Shoulder and Elbow Surgery, found that a single PRP injection produced significantly better pain, function, and sleep quality at 12 months compared to corticosteroid, with a treatment failure rate of 12% versus 30% in the cortisone group (p < 0.01). While the subacromial bursa is anatomically distinct from the olecranon bursa, both share the same bursal biology, chronic inflammation of a fluid-filled sac, and the PRP mechanism of action targets that shared biology.
A
2023 randomized trial of 180 patients with pes anserine bursitis comparing PRP, corticosteroid, and extracorporeal shockwave therapy3, published in Advances in Orthopedics, found that corticosteroid produced significantly better outcomes than PRP at both 1 week and 8 weeks. This study represents the only bursitis-specific head-to-head PRP versus cortisone comparison available in the literature, and its 8-week follow-up does not capture the longer-term outcomes where PRP's advantage over cortisone typically emerges in tendinopathy and joint research. The authors did not examine 6- or 12-month outcomes.
The honest summary: PRP has no dedicated RCT evidence for olecranon bursitis, and in the one available bursitis-specific PRP trial (pes anserine), cortisone outperformed PRP at 8 weeks. The clinical rationale for PRP in elbow bursitis rests on the subacromial bursitis data (superior 12-month outcomes), avoidance of cortisone's infection and skin complications in a superficial location, and use as a secondary option after cortisone has failed. Patients and providers should weigh this evidence gap honestly.
PRP vs. Cortisone for Elbow Bursitis
For most patients with acute or subacute olecranon bursitis after failed aspiration and conservative care, corticosteroid injection remains the standard first-line injection treatment. It reduces swelling and pain quickly, typically within 1–2 weeks, and most patients experience meaningful improvement. The important caveats are the elevated infection risk at this superficial location and the risk of skin atrophy with repeat injections.
PRP becomes a reasonable consideration in two scenarios: when cortisone has been tried without lasting benefit, or when a patient has had multiple cortisone injections and cumulative cortisone risks (skin changes, recurrent bursitis) make further steroid use undesirable. PRP works more slowly, improvement typically begins at 4–8 weeks, but does not carry cortisone's soft-tissue risks. For patients prioritizing safety over speed, or those with chronic recurrent bursitis, PRP is a biologically rational next step.
Who Is a Good Candidate?
PRP is most appropriate for patients with chronic or recurrent aseptic olecranon bursitis who have had aspiration and cortisone injection without lasting resolution, or who are concerned about further steroid exposure at this superficial site. Patients with significant bursal thickening and chronic wall changes on ultrasound, rather than simple acute fluid accumulation, are the most likely to benefit from a tissue-level treatment like PRP.
Septic (infected) bursitis must be excluded before any injection. The olecranon bursa is the most commonly infected bursa in the body, warmth, erythema, and systemic signs warrant aspiration and culture before proceeding with any injection therapy. Patients with gout or pseudogout causing bursitis should be treated appropriately for their underlying crystal arthropathy. Patients with large, fluctuant bursae that have not responded to multiple aspirations may be better served by surgical bursectomy.
What to Expect
Elbow bursitis PRP is performed as an outpatient procedure under ultrasound guidance. A blood draw is centrifuged to prepare the platelet-rich fraction, which is injected directly into the olecranon bursal space with real-time ultrasound confirming accurate placement. If significant fluid is present, aspiration may be performed immediately before PRP injection to decompress the bursa and maximize contact between the PRP and bursal wall. The procedure takes approximately 20–30 minutes.
Elbow rest and padding protection should continue for 2–4 weeks. Avoid direct pressure on the posterior elbow during recovery. Meaningful improvement in swelling and tenderness typically begins at 4–8 weeks. One injection is standard, with reassessment at 6–8 weeks. Recurrence is more likely if the underlying mechanical cause, habitual leaning on the elbow, repetitive pressure, is not addressed.
Sources
1. Kaur IP, Mughal MS, Aslam F, Schram J, Bansal P. Non-surgical treatment of aseptic olecranon bursitis: A systematic review. Reumatol Clin (Engl Ed). 2023;19(9):482-487. doi:10.1016/j.reumae.2023.05.004. PMID: 37945181.
2. Rossi LA, Brandariz R, Gorodischer T, et al. Subacromial injection of platelet-rich plasma provides greater improvement in pain and functional outcomes compared to corticosteroids at 1-year follow-up: a double-blinded randomized controlled trial. J Shoulder Elbow Surg. 2024;33(12):2563-2571. doi:10.1016/j.jse.2024.06.012. PMID: 39098382.
3. Gouda W, Abbas AS, Abdel-Aziz TM, et al. Comparing the Efficacy of Local Corticosteroid Injection, Platelet-Rich Plasma, and Extracorporeal Shockwave Therapy in the Treatment of Pes Anserine Bursitis: A Prospective, Randomized, Comparative Study. Adv Orthop. 2023;2023:5545520. doi:10.1155/2023/5545520. PMID: 37810418.
This content is for educational purposes only and does not constitute medical advice. Consult a qualified healthcare provider before starting any treatment.